Thousands of home care workers provide services to seniors and people with disabilities across the state of Montana. While caregivers have served at the front lines of Covid-19 pandemic and are essential to helping seniors and people with disabilities remain in their own homes and communities, they continue to earn poverty wages, without access to healthcare benefits.
In 2019, the median wage per hour for Personal Care Aides’ (PCAs) in Montana was below the national median hourly wage of $12.15 and far below a living wage. Wages for non-union home care workers in the state have remained relatively stagnant over the even as food prices paid by urban consumers rose over 4% in just one year.
Connie Sharp, a caregiver from Glasgow with 30 years of experience, says, “Most of us are still living paycheck to paycheck, and some months it feels like we’re just treading water.”
Montana’s minimal training requirements in home care work fail to create a safe environment for caregivers, seniors, and people with disabilities. PCAs in Montana are only required to complete 16 hours of training and 8 additional hours annually, compared to the minimum 75 hours required for Certified Nurse Assistants (CNAs) who do similar work in a facility setting. Montana does not regulate curriculum training or standards for home care workers employed directly by clients under Medicaid. Consistent and adequate training is critical for ensuring caregivers’ safety while providing care, and for guaranteeing that their clients receive the highest quality services.

“I continue to do this work because my clients need me. It’s been very scary to work through the pandemic. Many of my clients and other caregivers ended up getting sick with COVID-19. If my client didn’t have a caregiver, she wouldn’t be able to put the hose on herself or get clean or get to the toilet.” — Celeste Thompson, Missoula, Montana
A strong workforce to meet the need of an aging population
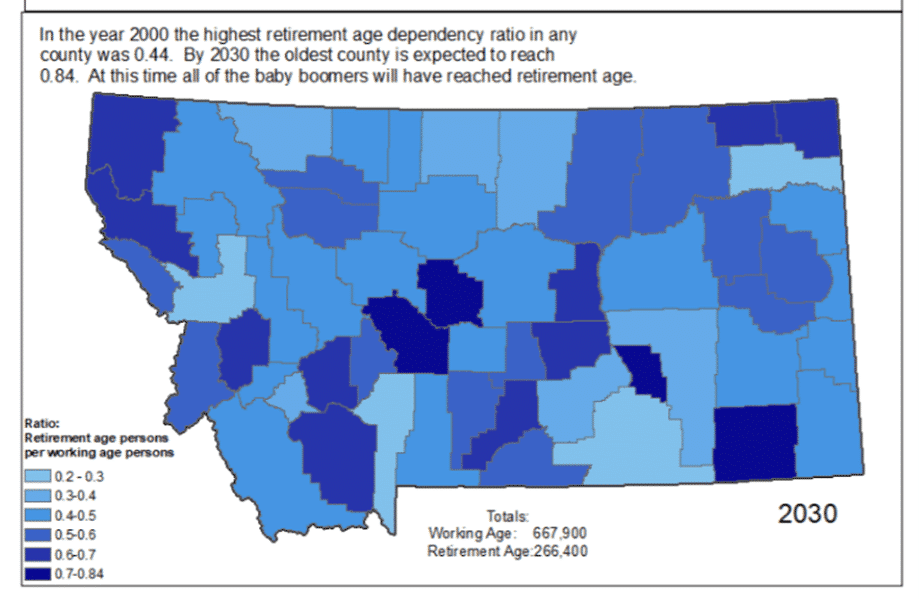
A strong care workforce is necessary to keep aging Montanans living in their own homes. Today, there are four people of working age for each elderly person in Montana; however, projections estimate that by 2030 the ratio will reduce to only two people of working age for each elderly person by 2030, creating a demand for caregivers who can meet increasingly complex care needs.
However, home care workers’ love and unwavering commitment for their clients still needs to be met with a living wage, benefits, and adequate training: in 2014, the direct care workforce in Montana, which includes personal care aides, had a turnover rate of 34.1%.
The Montana Healthcare Workforce Strategic Plan report recognizes that high turnover rates are linked to low wages, limited or no benefits, and inadequate training. Furthermore, the report establishes the state’s need to “work to ensure a living wage for all direct care workers, offer competitive wages and benefits that will reward tenure and enhancement of skills.”

Winnie Schafer, a home care worker and a member of the Sioux Tribe, highlights why workers stay on their jobs: “All caregivers would not be doing this if they didn’t love their jobs. I do this because I love my client, I love my job, and I love my union. If I didn’t, I would have quit years ago.”
Building a strong home care workforce that Montana’s economy needs
As other industries struggle with slow employment growth, home care jobs continue to grow. In Montana, personal care jobs are among the ten occupational groups with the highest annual projected occupation demand, and personal care aids’ opening job projections rank first among non-health care jobs within the healthcare industry (2018 -2020). PCAs are in every county in Montana — raising caregiver wages would be a boon to small businesses and local economies across the State.
Building a strong home care workforce is matter of racial and gender equity
Increasing wages, benefits, and training for home care workers is a matter of gender and racial equity. PHI latest demographic analysis of the direct workforce shows that “> representing 15% of all home care workers.
President Biden’s Plan to build a strong workforce: an opportunity for Montana
During his campaign, President Biden released the 21st Century Caregiving and Education Workforce plan. This document recognizes how critical care jobs are and outlines specific ways in which the federal government will support states’ efforts to strengthen their care infrastructure. The plan includes initiatives such as:
- Eliminating current waitlist for home and community services under Medicaid. This will allow more than 2,000 Montanans to access much-needed services.
- Giving states the option to transform their home and community-based care services waivers into state plan options with an enhanced federal match to increase home care workers’ wages and access to benefits.
- Investing in high-quality training and education programs for home care workers that lead to a certificate, as well as ongoing, job-embedded training and professional development.
- Ensuring home care workers have a way to organize, unionize, and collectively bargain.
Caregiving can be a good union job: the Washington State example
Building a care infrastructure capable of meeting the challenges of an aging population in Montana is possible. The state of Washington has built a strong home care workforce, including:
- A strong partnership with a overwhelmingly unionized workforce
- Starting wage of at least $17 per hour by 2023
- Comprehensive health insurance for $25 a month
- Training requirements similar to a CNA, including certification

